Menopause and Neurofeedback Training
Quick Navigation
Menopause can have adverse cognitive and mental health symptoms.
Neurofeedback training has been shown to be an effective, non-invasive, medication-free treatment for many of these.
It is a complementary therapy and evidence presented is based on general applicability, rather than being menopause-specific.
The menopausal transition is often accompanied by mood, memory and sleep issues.
Managing symptoms becomes important to avoid cumulative effects resulting in cognitive impairments.
Symptoms experienced during menopause include:
– weight gain and body awareness issues
– anxiety
– depression
– sexual dysfunction and impaired sense of self
– sleep disturbance
– brain fog: attention and working memory issues
– vasomotor irregularities: hot flashes, night sweats
Personalised Brain Training for Menopausal Symptoms
Personalised Brain Training aims to restore a healthy sense of self by working on brain areas that are core to our individuality, and addressing areas contributing towards anxiety, mood regulation, sleep, memory and physiological self-regulation.
The process is enjoyable – while watching a movie, we obtain a real-time measurement of a particular brain area’s performance. Feedback is given via small changes in volume, which our preconscious mind understands and uses to adjust it’s behaviour, thus learning to be more efficient. The result is a feeling of calm and self-assurance, with improvements in focus, motivation and sleep. Responsiveness can usually be assessed within a few sessions.
Neurofeedback for Various Symptoms
A brain map lets us look into our brain – how the different parts communicate with eath other. With neurofeedback, we can train optimal integration.
The following tabs describe how Personalised Brain Training can help resolve many mental health issues in a holistic, non-invasive and medication-free manner.
(Scroll down on mobile)
ADHD, Focus & Planning
ADHD as defined in the DSM-V can comprise a variety of different behaviour components, expressed in different magnitudes. Motivational, focus and planning, energetic, social behavioural, motor, learning and language and speech issues (e.g. dyslexia / dyscalculia) are included, and often comorbid with mood control, sleep, anger, rage, impulse control and aggression. Some are more prononounced than others, achieving sub-clinical manifestations for other diagnoses, and the picture soon becomes more complex.
With a brain map, we can assess vulnerability to a host of other possible issues, and then address these with neurofeedback training in a personalised manner. Furthermore, we have a chance at promoting structural improvements, such as prefrontal brain maturity. The core issue of ADHD, Distractibility, is dealt with here:
Focus and Productivity have three core components:
– Concentration
– Planning and Organisation
– Motivation
Each of these three components is governed by a different brain area. When one or more of these regions is dysrhythmic, we are vulnerable to focus issues.
– Planning and Organisation: understanding goals, working back to the present and structuring a workflow conducive to achievement, seeing the bigger picture and dividing projects into tasks, prioritising these and being flexible.
The ability to form an overview of the task at hand, break this down into smaller, manageable steps, and sequence these accordingly, can be trained.
– Concentration: the ability not to be distracted and maintain attention on the relevant task at hand. Distractibility is a function of spatial awareness, and there are brain areas dedicated to this task. When they are dysrythmic, we become easily distracted.
– Motivation: having sufficient drive, optimism, persistence and endurance to implement plans and overcome setbacks. Self-esteem, an understanding of one’s own strengths and weaknesses, and the ability to self-soothe, that is, to rationalise thoughts, are key to this.
Researchers conclude that neurofeedback training can be considered “Efficaceous and Specific” (Level 5) for ADD / ADHD. Neurofeedback training was shown to produce significant improvement in attentiveness and impulse control. It was shown to produce outcomes equivalent to those obtained with stimulant drugs. The effects were shown to be long lasting.
Neurofeedback and ADHD Medication
We have successfully helped children and teenagers reduce or discontinue stimulant medication treatment of ADHD where this has become undesirable, under supervision of the prescribing entity.
Individuals may offer motivations to change stimulant medication use to alternate forms of therapy, including ambiguity concerning long-term use and reduction of symptom-severity effectiveness at the cost of growth (height). Many are considered “prohibited substance” in competitive sports, being listed as Schedule II / Class B substances when obtained without prescription. Possible sleep problems are documented.
There appears to be a range of conclusions in studies regarding the effect of psychostimulants used to treat ADHD on mood, anxiety, emotional reactivity, substance abuse, psychiatric conditions, cardiovascular implications, tics and other dyskenisias, among other, and these vary considerably in sample size, duration and scope.
A study with over 130 participants showed that neurofeedback can be used effectively in combination with pharmacological treatment, enhancing results.
See here for more information.
Research on Neurofeedback and ADHD
Neurofeedback training for ADHD is evidence based and produces lasting results:
Attention deficit: Efficacy is well-documented – there are over 370 research reports on Neurofeedback and ADHD on PubMed.
In line with AAPB and ISNR guidelines for rating clinical efficacy, neurofeedback can be considered “Efficacious and Specific”, the highest level (5), with a large effect size for inattention and impulsivity in this study.
A large-scale study showed that neurofeedback is effective in remediating attentional dysfunction. Significant clinical improvement in one or more of attentiveness, impulse control, and response variability was observed in 85% of participants after 20-40 training sessions.
Impulse control and attention improved through neurofeedback training, producing “patient outcomes equivalent to those obtained with stimulant drugs”
Neurofeedback “appears to have more durable treatment effects, for at least 6 months following treatment.”
Neurofeedback was shown to be an effective method to enhance cognitive deficits, reduce ADHD symptoms and behaviour problems in children. The effect was maintained in a follow-up six months later.
There are numerous academic studies confirming the efficacy of EEG biofeedback (another name for neurofeedback) with sustained performance gains.
The American Academy of Pediatrics bases its conclusion that there are “no significant contraindications” to its use on these studies.
ILF / Othmer Method neurofeedback training was shown to reduce ADHD symptoms, specifically distractibility and impulsiveness, in a study involving 251 children over a course of 30 neurofeedback sessions.
Training specific brain areassuccessfully activated error monitoring networks in ADHD patients, associated with symptom improvements. Dynamic functional connectivity was found to be maintained in a follow-up 11 months later.
Another study attested improved response control and attention in ADHD post Neurofeedback.
Mood regulation and Motivation: see here
Working Memory: see here
Sense of Self: With Personalised Brain Training, we work on the Default Mode Network, the neural basis of self.
Challenging Behaviour, Anger, Aggression, Rage
Lack of mood regulation, self awareness, and inhibitory control contribute to anger management and behavioural issues. These complicated behaviour patterns have a neural basis and vary by individual. With a Kaiser Neuromap we can detect vulnerabilities and train these with neurofeedback.
Excessive obstinacy, misunderstanding social cues and general overwhelm and anxiety are frequent characteristics of autistic children. With neurofeedback training, we have had success in remediating these symptoms.
Multiple brain areas contribute to impulsive aggression, self-fuelling rage, physiological arousal, ‘acting out’ and conversely calming down and rationally understanding one’s behaviour and even showing regret, remorse, understanding and insight, or not as the case may be.
A Kaiser Neuromap shows us possible vulnerabilities to such behaviour patterns, and can help us form a more nuanced understanding of a person’s preconscious drivers, that is, their ‘wiring’. There are multiple contributors which we can address:
– impulsive aggression, e.g. in response to being denied something
– rage, a continued unconsolable stage
– lack of empathy or understanding of others’ feelings
– inability to see different perspectives
– turn taking, self/other differentiation, shared authority
– monitoring and understanding consequences of actions
With neurofeedback training we can work on these preconscious processes, which occur before a person is able to apply conscious control or inhibition. The aim is to reduce or eliminate the person’s propensity to exhibit such adverse and undesirable behaviour in the first place, freeing up the mind to enjoy the moment in constructive synchrony with others.
Neurofeedback helps us stabilise the Default Mode Network, and reduce impulsive aggression and physiological arousal control. We have seen success within a few sessions in clients from 8-15 years of age.
Anxiety and Fear
There are many manifestations of anxiety, including social anxiety, panic attacks, excess body awareness (body dysmorphia), emotional hypersensitivity, fears and phobias. Autistic children generally present with a variety of these, all contributing towards an energy-consuming heightened state of vigilance. Stress and defensive behaviour results.
Neurofeedback is an established, evidence-based treatment for anxiety.
It was found that neurofeedback training for anxiety and depression “results in enduring improvements approximately 80% of the time”
Confidence and social integration tend to improve accordingly, resulting in a positive feedback loop that helps shape new trajectories.
A brain map will reveal overactivity of brain areas responsible for monitoring consequences of actions (timidity, general fright and reticence); watching out for an abuser (bully); body and face awareness; and excessive self-monitoring. This helps us understand the potential presence of real threats and fear factors. We can also detect possible tendencies to develop unhealthy body awareness. Neurofeedback training lets us address this issues.

There are multiple types of anxiety, each correlating with one or more brain areas being dysrhythmic:
Sensory overload: our brain interprets all sensory stimulus as directed to ourselves. We lose the ability to discern what is directed at us, and which matters or interactions are of no concern to us. This sets us up for panic attacks and ultimately psychosis. It also means we become singular in our perspective, unable to take on other points of view
Loss of narrative: Our episodic understanding of the situation, how we got there and what happens next, is impaired, and we are unsure of where we are and where we’re going. This hyperactivates our amygdala, and the sensation is highly emotional
Auditory sensitivity: we become prone to overly interpreting the emotional content of words and sounds, creating an air of prickliness and pushing people away without knowing it
Social anxiety: misunderstanding social complexities, social emotions and dynamics in a situation with others
Hypervigilance: as a result of avoiding a bully or abuser
Activation: Our ARAS is responsible for setting the right level of physiological arousal, or wakefulness, for the situation, and to remain stable there. When this is on overdrive, we are pushed further into fight-or-flight mode than necessary, thus heightening sensory sensitivity. Panic attacks are an extreme manifestation. Our ability to calm down quickly is reduced.
Trauma: an inability to self-nurture – creating an emotional safe-space around us – and self-soothe – being able to talk ourselves down rationally from a situation, thus resulting in mood instability. This can also manifest in dissociation and heightened pain perception. We ruminate about the past and worry about the future, instead of being able to enjoy the present.
Intrusive thoughts: Self-criticism overshadows motivation and confidence, and we become self-aware and distracted by negative thoughts and feelings. Some use acquired habits to distract from this. Others become attached to the reward circuitry triggered, and sustained by feeding obstructive, self-deprecating thought content. Our confidence, motivation and social interaction suffer as a result.
Evidence: Neurofeedback for Anxiety
The effectiveness of neurofeedback training for anxiety was first recorded four decades ago in 1978. Since then, there have been over 120 peer-reviewed research papers published on neurofeedback and anxiety. Academic interest in this application of neurofeedback has picked up notably during the last three years.
Dr. Corydon Hammond finds in his 2005 paper, “Neurofeedback Treatment of Depression and Anxiety” that neurofeedback training results in “enduring improvements approximately 80% of the time”, with most perceiving a difference after between three and six sessions; a “very significant improvement” after 10-12 sessions, and more so after over 20 sessions.
Improving emotional regulation with neurofeedback represents a “novel intervention to control anxiety”. Just a single session resulted in a statistically significant improvement in anxiety.
Contamination anxiety was improved in a lasting way in this study .
Twenty sessions of neurofeedback training led to a significant improvement in sleep, anxiety and depression evaluations. The same disorders plus inattention showed significant improvements when conducting ten or more sessions in a naturalistic setting. Anxiety was reduced in Canadian Aboriginals during seven days of two hour training. Fifteen sessions reduced GAD symptoms.
Neurofeedback improved depressive symptoms in Major Depressive Disorder (MDD) patients, with significant decrease in anxiety and clinical illness severity noted as a result of the training. Cognitive depression was reduced here. Anhedonia and comorbid anxiety in MDD where also improved in this recent study. Increased happiness ratings and decrease in anxiety was documented with related increased activity in specific brain areas.
Post-operative depression and anxiety, pain, difficulties sleeping and attention and memory problems were resolved in 20 neurofeedback sessions. The 45-year old female was able to return to work subsequently. Postcancer cognitive impairment (PCCI) sufferers (a substantial subset of breast cancer survivors) found strongly significant reduction in anxiety, as well as somatisation and depression, after twenty neurofeedback sessions. Anxiety, as well as depression and tinnitus were greatly reduced during stroke rehabilitation, plus improvement in speech fluency, word finding, balance and coordination, attention and concentration.
Ten neurofeedback sessions improved symptoms of pain and fatigue, anxiety and depression in fybromyalgia patients. Neurofeedback was also found to reach maximum effect within four weeks.
Multiple Sclerosis sufferers saw depression, fatigue and anxiety reduced, and the results were maintained at a 2-month follow-up.
Alpha Theta neurofeedback training reduced anxiety in competitive ballroom dancers, as well as increasing cognitive creativity.
Neurofeedback provided benefit to high functioning ASD with regard to anxiety.
Alcohol Dependence Syndrome patients found a significant reduction in cognitive deficits, anxiety and depression; noticeable improvement in memory and neurological functioning, and significant reduction in alcohol intake on follow-up. Impulsivity, anxiety and depression were improved in long-term abstinent delinquents. Sharp reductions in self-assessed depression were found in alcoholic outpatients, as well as reduction in anxiety, after twenty Alpha-Theta sessions.
The physical basis of how neurofeedback training can be applied to reduce maladaptive rumination and anxiety was confirmed here.
Neurofeedback for Autism
Autism is a spectrum disorder characterised by social integration issues and developmental delays that can be both physical and emotional. With a Kaiser Neuromap we can identify individual weaknesses, and train these with Personalised Brain Training in a non-invasive, medication-free manner. Improvements are evidence-based and impressive.
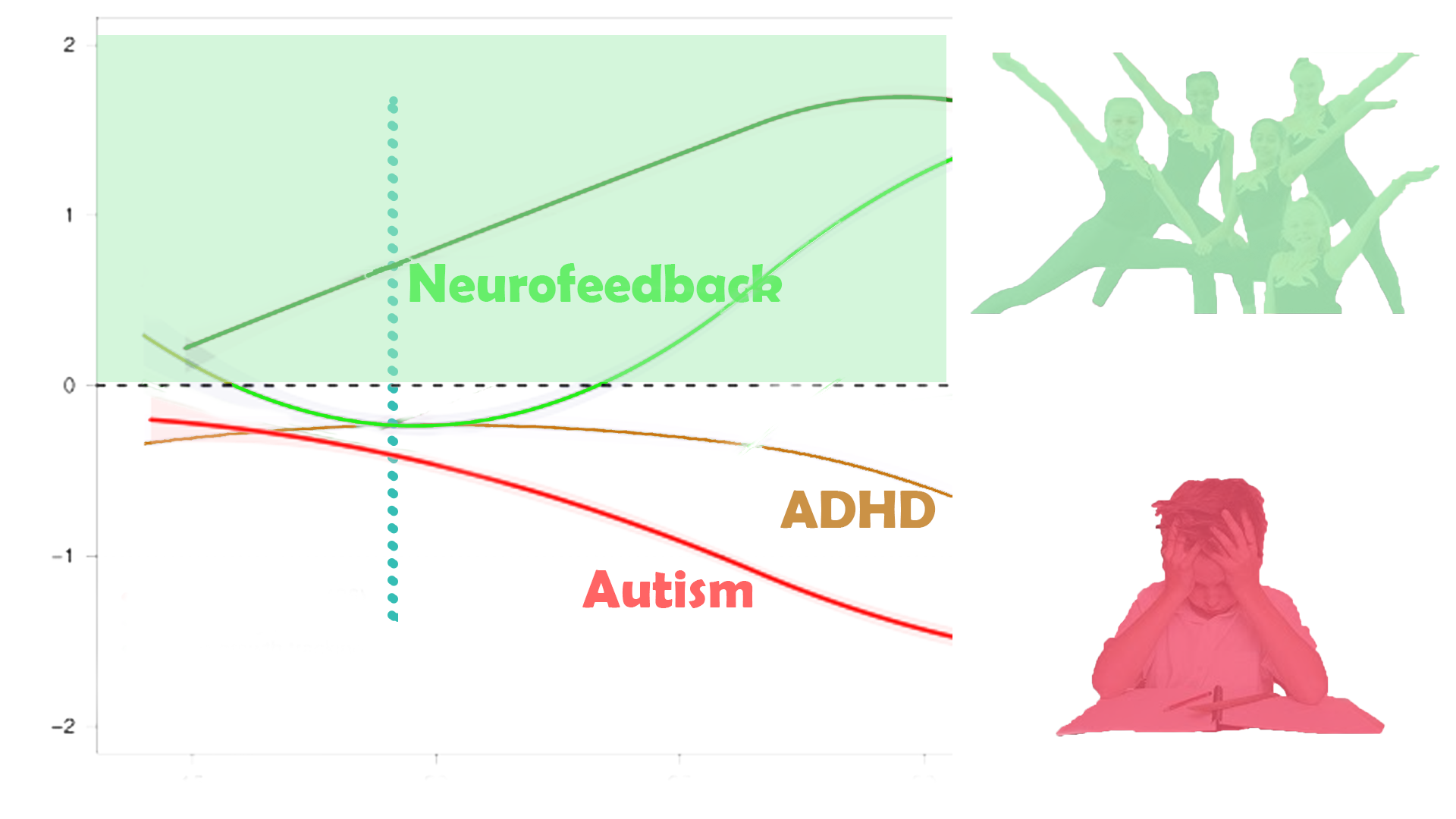
There are distinct brain areas that interpret the respective sensory input, and through various convergent processing stages – multi-modal association areas – the brain constructs a scene, and understands where we are with respect to our environment. When any of these brain areas becomes dysrhythmic, our interpretation becomes distorted, for example, we can become hyper- or hyposensitive, as is seen in various symptoms of autism.
With neurofeedback, we can train the brain areas relevant for efficient sensory processing and integration. Personalised Brain Training uses the most advanced qEEG brain map interpretation method to form an individualised training plan. Our neurofeedback method applies the most effective training protocols with an enjoyable feedback process, watching movies of choice.

Sensory processing is a well-researched process that involves many dedicated brain areas, and their interaction to produce an impression of our environment, and how it relates to us. Higher integration of ensuing awareness leads us into the realm of “what is consciousness”:
Science shows that our brain is engaged in a constant process of modelling, or predicting, our environment, both with regard to space and time. It does so on the basis of previous sensory information, as well as recent and consolidated memory. Predictions are then matched with reality, and the process begins again. This is an important distinction from the idea that we are merely reacting to our sensory input. It introduces the theory that we essentially anticipate the next moment, and then update our model of our environment, continually.
Autism can be viewed as an impaired capacity to efficiently engage in this predictive process. The theory easily explains the insistence on sameness and inflexibility with regard to changing routines, embracing novelty, interacting with moving objects, reduced appreciation of humour and even Theory of Mind, which is essentially the creation of a model of another person in one’s own mind. An unpredictable world becomes overwhelming, explaining the fear and anxiety we so often witness with the condition, and resorting to self-stimulation (stimming) is an anxiolytic response. As a result of reduced modelling and predictive capacity, repetition is favoured, and this can turn into a strength as replicative behaviours enhance certain skills or narrow areas of focus.
We can think of autism as brain dysregulation in multiple functional areas. This results in many comorbidities, which we implicitly address with neurofeedback training as part of a holistic approach.
Some of the challenges we have seen to improve with neurofeedback training include:
– lack of bodily awareness, motion control and speech, spatial awareness
– an inability to express, understand and convey emotions and physical needs
– increased frustration at not being understood, whether on a basic survival needs level or in more emotional / intellectual areas
– impulsive aggression, potentially morphing into self-fuelling rage and violent behaviour, sometimes self-directed
– perceived lack of empathy and regard for the needs of others
– generally being ‘misunderstood’, to the detriment being able to fully develop strengths and talents
With neurofeedback training, we can address these ultimately self-harming divergences and bring out the incredible potential in all of us.
Neurofeedback training has been shown to be a safe, feasible, and effective therapy approach to Autism Spectrum Disorder across all ages.
Multiple studies confirm:
– improved cognitive function in social, thought and attention domains
– improved cognitive flexibility
– lasting improvement in executive function, working memory and processing speed
– improved facial recognition
– better behaviour, including being less aggressive, more cooperative and better at communication
– improved functional connectivity in the social brain regions
– a 40% reduction in ASD symptoms among 89% of participants, and associated changes in cerebral functional connectivity
– lasting improvement in ACC / DMN flexibility, crucially linked to Theory of Mind
– significant improvements in general and non-verbal communication and social interaction
– lasting, and increasing improvements past the training period, in attention control, cognitive flexibility, planning, communication and social interaction
A 9 point improvement in IQ was reported in a large-scale study, alongside decreased ASD symptoms including attention, anxiety, aprosodias, social functioning, as well as academic and intellectual functioning.
Sensorimotor behaviour (posturography) improved in children.
Neurofeedback training has proven calming effects.
Research evidence for comorbidities, e.g. ADHD, dyslexia, depression, anxiety, seizures, sleep and behaviour is shown under the relevant tabs below.
Emotional Balance is a core necessity for enduring, controlling and dominating the rollercoaster that competition provides.
Neurofeedback is an established method for treating anxiety.
Athletic training and competition involves a lot of changing gears when it comes to physiological arousal. From warm-up to competing, cooling down and waiting for the next stage, gearing up again and performing, and repeating this possibly multiple times in a day or session, flexibility and stability is key.
We can train our brain to be more flexible and stable, in particular with respect to having the right, and steady level of physiological arousal for the situation.
Fears, setbacks and even easy wins can impair our judgement and performance. Having a strong sense of emotional safety, and the ability to self-soothe, are instrumental in ensuring reliable performance.
Neurofeedback takes a holistic approach to emotional balance.

Over-attentive with regard to bodies, shapes and faces, and excessive monitoring of our own in relation to others, our self-confidence and social interactions suffer. There are neural correlates for this which we can train.
Studies have shown that there are neurological differences in people with Body Dysmorphia Disorder. By identifying neuromarkers, we can assess vulnerability using a qEEG brain map (Kaiser Neuromap), and then train the affected brain areas accordingly using neurofeedback.
The condition affects higher order visual processing areas, which relates to the emphasis on face and body recognition and the over-attention to detail.
Also, prefrontal areas pertaining to self-monitoring, risk-taking and empathy are activated differently in BDD.
Sub-cortical structures involved in reward processing see similar activations.
BDD has many comorbidities, including anxieties, social phobia, depression and OCD. Impulsive aggression (violence) and suicidal ideation are also common, as are intrusive thoughts.
From our experience, these issues, among other, show up as vulnerabilities on a Kaiser Neuromap, and we have successfully resolved body dysmorphia issues in clients using Personalised Brain Training, besides many other comorbidities.
Traumatic Brain Injury & Concussion
Traumatic Brain Injury (TBI) is another application of neurofeedback training.
We have found neurofeedback to be highly effective in assisting physical rehabilitation. With a Kaiser Neuromap, we can detect areas of hypometabolism that respond hemodynamically with neurofeedback training. There are neuromarkers for mTBI, as well as Alzheimer’s Disease, though these are non-specific (necessary, not sufficient conditions) and should not be seen as diagnosis. General (rather than focal) lesions in neurodegenerative conditions appear to form first in the corpus callosum, a fibre bundle linking the two brain hemispheres; altered functional connectivity has been visible there on a brain map too, in our experience, at an early stage.
There is evidence that neurofeedback supports myelination, improving the important sheathing of axons, which is a critical part of the physical recovery process.
With a brain map, we can detect areas of hypometabolism, some of which are characteristic of mTBI / concussion. Using the most advanced neurofeedback protocols, we have reversed these, indicating the positive hemodynamic effects of neurofeedback training.
Pain perception has neural correlates – there are brain areas that govern our attentiveness to the signs our bodies are giving us.
In the first instance, these signs are real messages that something is wrong and needs dealing with. Medical attention should provide solutions to this.
Sometimes, pain perception can become irrational in this context, and with neurofeedback training we can help the brain establish a more reasonable approach to interpreting such stimulus.
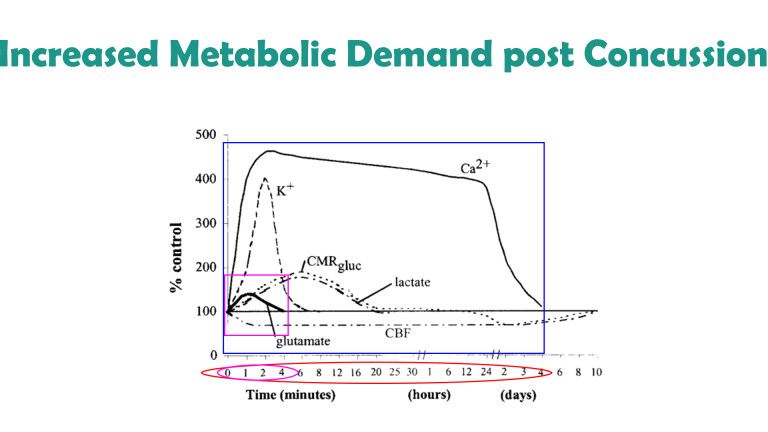
Immediately following concussion / mTBI, there is an increased demand on energy (glutamate) in the brain, at the same time as cerebral blood flow is constrained.
This effect is most pronounced during the first four minutes following impact; other neuromodulatory impairments last for days, and it is estimated that cerebral blood flow is only normalised after around ten days. The blood brain barrier is temporarily disrupted in the first few minutes leading to a complex inflammatory response in the hours and days following injury, and microglia can remain activated for many years.
There are numerous neuromarkers of mTBI, ranging from reduced prefrontal activation to impaired Default Mode Network functionality; while these are non-specific – necessary, but not sufficient conditions – some are highly unusual and show up on a Kaiser Neuromap. With neurofeedback, we can train these, while restoring general functionality of our neural basis of self (the Default Mode Network). We have seen impressive recoveries, both with regard to client feedback and before/after brain maps.
Concussion / mTBI increased the risk of Alzheimer’s Disease by 50% and shares similar mechanisms of promoting tau / amyloid pathology. TBI also increases the risk of Parkinson’s Disease and is capable of producing a prion-like spread of self-seeding proteinopathy. Moderate to severe TBI adds around five years to measured brain age, relative to chronological age.
Research on Neurofeedback for Rehabilitation
– Alpha-Theta neurofeedback training has a “beneficial effect on symptom reduction as well as perceived stress. It also has a beneficial effect on levels of serum cortisol” involving a significant reduction during acute recovery
– neurofeedback training was shown to be effective with Postconcussion Syndrome (PCS)
– efficaceous treatment for chronic posttraumatic headache sustained in military service
– neurofeedback therapy showed significant changes in structural and functional connectivity in young TBI patients, with cognitive scores and concussion symptoms improving significantly
– neurofeedback is shown to be an effective intervention for auditory memory
– deemed “probably an excellent complementary technique” that produced clear benefits in divided and sustained attention, visuospatial skills and the processing speed of motor-dependent tasks in persons with severe TBI
– beneficial outcomes in upper limb stroke rehabilitation
– neurofeedback training can lead to a learned modulation of brain signals with associated changes at both neural and behavioural level
– modulation of premotor cortex and associated motor control areas can be achieved with neurofeedback training
– improvements in TBI / PTSD in Vietnam Veterans across domains of cognition, pain, sleep, fatigue, mood/emotion, PTSD symptoms and overall activity levels
– patients report improvement in a wide range of neuropsychiatric symptoms in TBI following neurofeedback training
– result of 40 neurofeedback sessions included significant improvements in several motor tasks
The recent rugby player study by the Drake Foundation showed that 23% of players (10 out of 44) had axonal or diffuse vascular injury. This contrasted with athletes in non-collision sports.
Mild traumatic brain injuries are common in rugby, with an incidence rate of 20.4 per 1,000 player match hours (14.8 per 1000h in Australia).
In addition to mTBI, repeated head impacts can lead to neurodegeneration that becomes progressive. This increases the risk of dementia.
Trauma, (C-)PTSD
Trauma and abuse leave scars.
When the viability of our existence has been subjected to threat, our behaviour adapts. We become primed for hypervigilance, sensitive to triggers, and our physiology responds accordingly. A heightened sense of awareness now confers safety, and we can even become addicted to this.

Our brain keeps the score: Areas responsible for defence and vigilance are activated, even when there is no objective reason. Sensory stimulus is amplified, and we dedicate value energy resources to the monitoring of others’ intentions. Anxieties are rekindled, and the strain on our system leaves us exhausted while unable to switch off and effectively recuperate. Our focus and productivity drop, as does our self-esteem. We can feel detached from our bodies, dissociating. Our social capacity is impaired.
Neurofeedback helps us break this cycle: we equip the brain to get over it, to get on with it, re-establish our sense of self-worth, and the ability to constructively engage with our environment. We gain a healthy sense of detachment, which allows us to process the past more efficiently and look forward to the future.
With a brain map, we can identify which parts of our system are being particularly stressed. Neurofeedback training helps us bring these brain areas into better alignment.
Typical Symptoms of Trauma and PTSD
The first indication that we are experiencing trauma / PTSD is when we find ourselves not living in the present. Enjoyment of the moment and social interaction is clouded by constant ruminations about the past, and worries about the future. We are unable to ‘let go’, relax, and grasp opportunities as they present themselves in the Now.
We are plagued by intrusive thoughts that bring us back to events in the past, which needn’t even be related to a traumatic event, but which remind us of some inadequacy and amplify our self-doubt. Feelings of shame and guilt come into the picture as well, further eroding our self-confidence. “How can I be happy and enjoy this after what has happened?”. Similarly, our perception of the future is shrouded in worry and fearful anticipation. Uncertainty is our greatest foe, our perception of safety is unhinged by any doubt as to what could happen next.
The absence of a plan becomes a concern, the lack of clarity as to what’s around the corner a burden. Negativity associated with the past deprives us of hope. We are thus unable to see uncharted territories ahead as an opportunity, and much rather dwell on impending threats.
Indeed, our system is primed to protect us, and we are in survival mode. This process becomes self-feeding as we become addicted to the hyper-arousal our sense of fear induces. Our sense of joy and looking forward to fun becomes clouded to the extent we forget and no longer yearn it. Detachment sets in, further isolating us from feelings that previously motivated us. This process can even start slow and subtly, yet the cycle is self-fulfilling and deprives us of the necessary perspective to break and get out.
In Personalised Brain Training, our definition of trauma is wider. We include for example perceived loss of social standing, which can be either the cause or the consequence of a traumatic event or development. The perceived loss of social position results in us feeling judged. We become hypersensitive to how people approach us, talk to us, deal with us.
This is a subjective concept, as it should be, given that trauma should be recognised as an issue of perception by the affected person, rather than a concept being ‘awarded’ by an unrelated party, though external affirmation can help and medical advice should be sought in any event. As humans, social recognition is a critical component of our biological drive to propagate. Attraction relies on this, which ultimately leads to bonding.
Consequently, there are numerous brain areas devoted to, or involved in, the assessment of our position with regard to others. When our self-perception is assailed, or even the viability of our self is questioned, we are naturally shaken. Various brain areas become dysrhythmic. These include areas responsible for our body control and awareness, and many therapies focus on engaging the body and somatosensory system with a view to inducing cerebral changes.
However, this is only a part of the picture – there are many, arguably more powerful neuronal centres in the brain that are affected by trauma, and with a Kaiser Neuromap and Default Network Training (together, Personalised Brain Training), we can assess the issues more accurately, completely and efficiently, as well as then successfully training the brain to overcome trauma and setting ourselves on course for a positive trajectory.
Another consequence of trauma is that we may feel unable to rationally assert a sense of safety. This is different to self-nurture, or an emotional sense of safety. When we are unable to talk ourselves down from a situation we lose the ability to effectively regulate our moods, to switch off when we need to, and ultimately can become excessively paranoid.
There are neural correlates for this behaviour, and we can asses this with a Kaiser Neuromap. Safety and assurance are core needs we are programmed to seek to fulfil. Authority and role models help us in this quest. When we become dysregulated in our ability to self-soothe, we are also compromised in our ability to find paternal guidance. As a result, we tend to over-idolise figures who seemingly exude strength and power, or disobey completely and become unnecessarily rebellious – both immature behaviour patterns. Resetting this balance is crucial to achieving calming, regulated emotions, reduced hypervigilance and controlling impulsiveness. Personalised Brain Training lets us achieve this.
When hypervigilance persists untreated, we face further problems.
Physically, our heart beats faster and harder, more of the time, which is a clear stress on our system.
Mentally, we become prone to developing intrusive thoughts, even when we are able to relax, and more so when we are stressed, where these can take on third-person character, a voice in our head. This can have a destabilising effect, not least because we are now spending energy ‘defeating’ other perspectives we are internally engaged with, and thus distracting us from the ‘now’. Being on hyper-alert can also make us more susceptible to feeling relational to sensory input, in that we feel that everything is directed at us, which can set us up for psychosis.
As we lose our ability to enjoy the moment, our social interactions suffer. Exercising our social brain keeps us alive and forms the basis for sound mental health. Our brains are adaptive, and we need to provide stimulus to maintain connections and sustain flexibility. Isolation deprives us of many necessary exercises. For example, brain areas that deal with face recognition also respond to affective interactions and the ability to discriminate between emotional content of faces. We need to keep training these brain areas through social interaction in order to maintain emotional recognition – it is not a surprise that perpetual mask-wearing heightens our social anxiety (aside from adverse physical effects).
Social recognition, a key component of our biological need to attract and bond, is driven by sensory interpretations. Again, we need to exercise brain areas that contribute to this, including language and speech generation and comprehension, auditory sensitivity, and monitoring rewards for actions, both directly and vicariously. Our mirror neuron system contributes towards learning from others’ mistakes or examples, and consequently the storage of social rules necessary for constructive functioning in a society.
Inclusion is imperative to establishing a healthy self-image or sense of self. This in turn is crucial to forming stable relationships with friends, family and forming healthy alliances necessary for personal and professional progression. When we lose our sense of belonging to a group or cause, we may become unstable in our self-perception and our relationships with others. The effect may snowball into perceptions of abandonment, feelings of emptiness and dissociation; this in turn correlates with mood dysregulation, impulsive and often dangerous behaviours, intrusive thoughts and potential self-harm.
With Personalised Brain Training, we can assess vulnerability to these traits as they manifest in functional brain area dysrhythmia that shows in a Kaiser Neuromap; with Default Network Training, an advanced form of neurofeedback, we can train these brain areas and networks in a holistic manner to help re-establish balance. This enables us to reconnect with our environment and re-enter a positive feedback loop.
Sleep is adversely affected by trauma. First, the mind needs to ‘let go’ in order to enter deeper sleep cycles, which is a challenge for many. Excessive rumination and intrusive thoughts can hinder this, as does the loss of our ability to rationally calm ourselves down. The depth of our sleep is governed by our ability to self-nurture and create an emotional ‘safe space’. Homeostasis during various sleep stages is governed by other parts of our brain, some still involving the cortex. With a Kaiser Neuromap we can detect dysrhythmia in the relevant brain areas and train these accordingly with Default Network Training (together, Personalised Brain Training).
Focus and organisation suffers as a consequence of sleep issues. This time, different brain areas are affected, which we can also train. When we are unable to concentrate and produce our best output, we become demotivated and our mood and sense of self suffer. Again, there are brain areas responsible for these aspects of being, for which we can again detect dysrhythmia and provide neurofeedback training. The process is holistic – many components have to work together effectively for us to function optimally.
Mood regulation suffers when we lose social integration, sleep and focus. Neurofeedback training found to significantly help 80% of people with depression by aiming to restore motivation, improving sleep and focus, and reducing anxiety.
There are numerous potential cortical contributors to depression, and with a brain map we can see vulnerabilities.
Neurofeedback training lets us address these as well as establish a generally improved sense of well-being in a holistic manner. he positive effects of neurofeedback training have been shown to be lasting. Neurofeedback is non-invasive and medication-free.
There are multiple types of anxiety, each correlating with one or more brain areas being dysrhythmic:
- Social anxiety: When we’re in a situation with other people and our understanding of the social dynamics and complexities is overwhelmed.
- Sensory overload: our brain interprets all sensory stimulus as directed to ourselves. We lose the ability to discern what is directed at us, and which matters or interactions are of no concern to us. This sets us up for panic attacks and ultimately psychosis. It also means we become singular in our perspective, unable to take on other points of view
- Loss of narrative: Our episodic understanding of the situation, how we got there and what happens next, is impaired, and we are unsure of where we are and where we’re going. This hyperactivates our amygdala, and the sensation is highly emotional
- Auditory sensitivity: we become prone to overly interpreting the emotional content of words and sounds, creating an air of prickliness and pushing people away without knowing it
- Activation: Our ARAS is responsible for setting the right level of physiological arousal, or wakefulness, for the situation, and to remain stable there. When this is on overdrive, we are pushed further into fight-or-flight mode than necessary, thus heightening sensory sensitivity. Panic attacks are an extreme manifestation.
- Trauma: an inability to self-nurture – creating an emotional safe-space around us – and self-soothe – being able to talk ourselves down rationally from a situation, thus resulting in mood instability. This can also manifest in dissociation and heightened pain perception. We ruminate about the past and worry about the future, instead of being able to enjoy the present.
- Intrusive thoughts: Self-criticism overshadows motivation and confidence, and we become self-aware and distracted by negative thoughts and feelings. Some use acquired habits to distract from this. Our confidence, motivation and social interaction suffer as a result.
The primary issue of trauma affects brain areas that are activated during empathy and forgiveness. With these two qualities impaired, our emotional life suffers, as do our social capacities. With neurofeedback training, we can restore functionality of these brain areas. Another reason this is important is because we do not want to become oppressors ourselves. As we lose our sense of emotional investment in our surroundings, we become careless with regard to others’ feelings and needs.
Implicitly, we are now capable of unintended yet real behaviour patterns that can harm others, as we become deaf to feedback. Not only has trauma affected us, it now makes us perpetrators that pass it on.
Besides reduced social interaction and a less meaningful emotional life that is now more self-centred – and with the wrong type of therapy, becomes self-indulgent and self-perpetuating – we can experience a physical withdrawal from our environment. Dissociation can be momentary and intense, or subtle and ongoing to the extent that we are not even cognisant of it. Either way, our bodies retreat from sensations, analogous to our emotional withdrawal.
Many therapies aim to revive our sense of ownership of our bodies, and thus ultimately our life and future, by training our body awareness in various ways. Realising that our bodies are steered by our mind, specifically our cortex, we can train the relevant brain areas that govern our body perception and movement execution.
Neurofeedback training effectively complements these approaches by directly treating the areas involved in perception and interaction with our surroundings.
One of the first manifestations of trauma is in our bodies. Aside from heightened physiological arousal, a form of paralysis can override our natural motions and postures. Stress, and pain ensue, which can often be felt all around the body. Fibromyalgia is a variant of this phenomenon, as are headaches, chest pains, and chronic fatigue.
There are many techniques for combating this form of physical dissociation. Neurofeedback complements these by training the brain areas that instruct the body to behave in this undesirable way. It is a holistic approach, and we restore overall calming while providing the brain with rational and emotional capacity to overcome its challenges.
An inability to self-nurture – creating an emotional safe-space around us – and self-soothe – being able to talk ourselves down rationally from a situation, thus resulting in mood instability. This can also manifest in dissociation and heightened pain perception, fibromyalgia and chronic fatigue. We ruminate about the past and worry about the future, instead of being able to enjoy the present.
Our autonomic nervous system is primed to produce sympathetic nervous system responses, or fight-flight-freeze mode. This wears us down, as it is more energy intensive, our recuperation periods are shortened and we can even become used to the adrenalinergic buzz of being in hypervigilant overdrive. It becomes a safe space. Our pain perception is altered and fluctuates between numbness and hypersensitivity. Deprived of a ‘calm’ reference state, we become vulnerable to overattributing emotions to sensations.
Dissociation is another phenomenon that can ensue, and this can be subtle and paroxysmal. Engagement of defensive mechanisms is triggered pre-, or subconsciously. This can compromise our ability to rationally self-soothe – the role of our prefrontal cortex. Instead, our limbic system is primed. We also lose our emotional sense of safety. The integrity of our Default Mode Network is challenged, as is the natural transition between its activation and that of the Task Positive Network. We are less able to regulate engagement with our environment and the neurological basis for our sense of self is under threat.
There are distinct brain areas regulating pain, physical sensations and our self-awareness, and we can train these with neurofeedback. We can also train brain areas with strong connections to sub-cortical structures that regulate our autonomic nervous system, including the amygdala and our reticular activating (or limbic) system. Our brain is ultimately in charge of trauma response, and with neurofeedback we can assess vulnerability to its various submodalities, and address these with training. This is evidence-based and effective.
Dyslexia
Dyslexia often presents together with ADD/ADHD and other behavioural issues. With a Kaiser Neuromap, we can assess vulnerabilities, and then train these with Personalised Brain Training.
Dyslexia is an impaired ability to understand written and printed words or phrases and affects 10-20% of the population in both males and females. The disorder can result in learning difficulties, poor academic performance, stigmatisation and ensuing behavioural issues.
While often classed as a disability, there are associated strengths: creativity, the ability to solve complex problems, unorthodox approaches to ideas and projects, and a more detached ability to apply logical thinking are some of these. Nonetheless, the condition can impair school and social functioning, slow maturation and significantly affect self-confidence and -esteem.
“Picked up a book and started reading! Unheard of before, I could never get her interested in reading for herself.” – Mother of Anna (9)

There are neural correlates with dyslexia which we can train with neurofeedback.
Reading and comprehension involves multiple brain areas as well as their seamless communication. We have Wernicke’s area for comprehension, and Broca’s for speech generation. Additionally, there are regions involved in sequencing, visual recognition, focus and attention, and contextualisation or syntax recognition of subject matter along with various memory-related areas.
It is important to note that there are different types of dyslexia. A brain map shows us which brain areas are dysrhythmic.
With neurofeedback, we train brain areas involved in visual and auditory processing; memory; focus and attention; syntax and context; sequencing and organisation. We also train the connections between these areas. The approach is holistic: we work on core networks, and their integration with each other.
Research on Neurofeedback and Dyslexia
Research has shown that neurofeedback training can improve reading ability and phonolocigal awareness deficit in children with reading disabilities, as well as improvements in spelling.
For a summary of 18 neuroscientific research studies on language learning impairment produced until 2015, see here.
Fibromyalgia
Fibromyalgia is often linked to trauma and presents with other symptoms such as anxiety, mood dysregulation and sleep issues. Neurofeedback is an evidence-based treatment for many of these comorbidities.
The elusive source of pain in fibromyalgia can result in misdiagnosis, and often skepticism from medical professionals, compounded by a lack of specific treatment options. This can further erode the sufferer’s self confidence, as they are faced with doubt and misunderstanding. With neurofeedback, we take a holistic approach by stabilising the Default Mode Network, thus re-establishing a healthy sense of self; helping with exacerbating factors such as sleep and motivation issues, and anxieties. Neurofeedback has been shown to be effective in trauma and PTSD.
Fibromyalgia patients report significantly improved pain severity and interference, fibromyalgia symptom severity, sleep latency and sustained attention following eight weeks of neurofeedback training.
A separate study finds significant improvement in cognitive dysfunction, fatigue, pain, sleep, depression and overall activity level in fibromyalgia sufferers, further illustrating the debilitating comorbidities of this condition.
Fibromyalgia patients saw an 82% reduction of fatigue, depression and anxiety, and an increase in social and physical functioning; these effects were upheld. Another fibromyalgia study with different neurofeedback protocols achieved a 39% improvement, and another found a 55% improvement. Neurofeedback training improved functional connectivity in somatomotor areas leading to reduced impact of fibromyalgia and pain symptoms and improved quality of life.
Chronic pain sufferers of Spinal Chord Injury found immediate and lasting effects on pain intensity from neurofeedback training.
Self-criticism overshadows motivation and confidence, and we become self-aware and distracted by negative thoughts and feelings. Some use acquired habits to distract from this. Our confidence, motivation and social interaction suffer as a result.
Menopause
Menopause can have adverse cognitive and mental health symptoms. This is a particularly difficult time when raising children with strong emotional needs as they enter puberty contemporaneously. Ideally, we would like to be grounded and able to offer support while going through a transformative period ourselves.
Neurofeedback training has been shown to be an effective, non-invasive, medication-free treatment for many mental health issues precipitated or exacerbated by menopause..
It is a complementary therapy and evidence presented is based on general applicability, rather than being menopause-specific.
The menopausal transition is often accompanied by mood, memory and sleep issues.
Managing symptoms becomes important to avoid cumulative effects resulting in cognitive impairments.
Symptoms experienced during menopause include:
– weight gain and body awareness issues
– anxiety
– depression
– sexual dysfunction and impaired sense of self
– sleep disturbance
– brain fog: attention and working memory issues
– vasomotor irregularities: hot flashes, night sweats
Personalised Brain Training aims to restore a healthy sense of self by working on brain areas that are core to our individuality, and addressing areas contributing towards anxiety, mood regulation, sleep, memory and physiological self-regulation.
The process is enjoyable – while watching a movie, we obtain a real-time measurement of a particular brain area’s performance. Feedback is given via small changes in volume, which our preconscious mind understands and uses to adjust it’s behaviour, thus learning to be more efficient. The result is a feeling of calm and self-assurance, with improvements in focus, motivation and sleep. Responsiveness can usually be assessed within a few sessions.
Depression, Bipolar Disorder, Mood Regulation and Motivation
There are numerous contributors to depressive tendencies from a neural perspective. A brain map lets us identify possible cortical contributors, and we can train important neural hubs that affect our ability to regulate mood.
In this sense, neurofeedback is a next-generation treatment for depression. We seek to avoid reliance on medication, especially from an early age.
The effectiveness of neurofeedback training in treating depression is well-documented. Effects have been shown to be strong and lasting. Working on depression helps us re-establish our sense of safety in the world, and often correlates with our ability to fall asleep.
There are multiple contributors to Depression, and neurofeedback has been shown to help with each:
– mood regulation and stability
– motivation and productivity
– sleep and effective recuperation
With Personalised Brain Training we take a holistic approach: Key neural networks responsible for our sense of self, for focus and productivity, and for mood regulation are addressed during neurofeedback training. The process is non-invasive and medication free, as well as enjoyable as we use movies to embed the feedback.
Bipolar disorder affects one in five people with depression. Again, we can address brain areas responsible for maintaining stability, and help calming, particularly important during manic episodes, thus seeking to avoid psychosis. Also, given that more than two-thirds of bipolar disorder sufferers are misdiagnosed initially, identifying the presence of non-specific neuromarkers can aid (but not replace) the diagnosis process.
Examples for the Scientific Basis of Neurofeedback
The US National Library of Medicine records over 140 peer-reviewed research papers on neurofeedback and depression, with a significant recent rise in research attention to this non-invasive, drug-free treatment method. Here are some excerpts of the scientific evidence supporting neurofeedback for depression. Note the diversity of brain areas involved, suggesting that depression need not have a single nor consistent source, and the comorbidities often found:
Dr. Corydon Hammond finds in his 2005 paper, “Neurofeedback Treatment of Depression and Anxiety” that neurofeedback training results in “enduring improvements approximately 80% of the time”, with most perceiving a difference after between three and six sessions; a “very significant improvement” after 10-12 sessions, and more so after over 20 sessions.
Twenty sessions of neurofeedback training led to a significant improvement in sleep, anxiety and depression evaluations. The same disorders plus inattention showed significant improvements when conducting ten or more sessions in a naturalistic setting.
Neurofeedback improved depressive symptoms in Major Depressive Disorder (MDD) patients, with significant decrease in anxiety and clinical illness severity noted as a result of the training. Cognitive depression was reduced here. Anhedonia and comorbid anxiety in MDD were also improved in this recent study. Cognitive impairment during MDD is recognised and neurofeedback treatment advocated. Its effectiveness on a variety of cognitive functions in MDD such as working memory, attention and executive functions is established.
Neurofeedback is recognised as a next-generation treatment for Major Depressive Disorder.
Increased happiness ratings, mood improvements and decrease in anxiety was documented with related increased activity in specific brain areas. Cognitive-affective brain areas as neural targets for treating depression are recognised here, while higher-order visual areas are implicated in this study that recognises that neurofeedback training can reduce depressive symptoms by over 40%. Further success in treating MDD with comorbid anxiety symptoms was documented here, training specific brain areas.
Sub-threshold depression was improved in college students and recommended as an effective new way for college students to improve self-regulation of emotion.
Rumination, a maladaptive emotional-regulation strategy, was found to have a neurological basis that was successfully reduced while ameliorating depression. The tendency to preferentially attend to negative stimuli in the world and negative thoughts in mind during depression was found to be controllable with neurofeedback. Ruminative processes and avoidance when dealing with autobiographical memories were attributed to specific brain areas and recognised as contributing to Major Depressive Disorder, promoting neurofeedback training as a depression treatment. Similar brain areas when trained with neurofeedback resulted in improvements in self-esteem.
Training brain areas responsive to negative stimuli decreased negative cognitive biases in MDD, showing greater decrease in self-reported emotional response to negative scenes and self-descriptive adjectives. Neurofeedback training is also able to improve processing of positive stimuli in MDD patients. Another recent study achieved significant improvements in reducing the severity of depression and rumination in MDD training a different brain area. Lasting effects of reinforcement learning of better brain habits on rehabilitating emotion regulation in depression through neurofeedback were found. Depressive symptoms were alleviated consistently.
The treatment resistance of recurrent depression is linked to rigid negative self-representations during an identity formative period in adolescents, with potential lifetime repercussions. The study finds neurological evidence for which it recommends neurofeedback interventions. Significant and lasting improvements following neurofeedback training were discovered in another study on Treatment Resistant Depression (TRD). Significant reduction in depression symptoms were reported after four neurofeedback sessions in patients showing no response to current pharmacological or psychological therapies for depression.
Post-operative depression and anxiety, pain, difficulties sleeping and attention and memory problems were resolved in 20 neurofeedback sessions. The 45-year old female was able to return to work subsequently. Cancer patients found non-invasive, drug-free neurofeedback to ameliorate pain, fatigue, depression and sleep. Chronic Stroke victims found neurofeedback therapy to reduce anxiety and depression level while improving motor, verbal and cognitive skills.
Opiate addicts treated additionally with neurofeedback showed greater improvement in depression and somatic symptoms, and relief from withdrawal, as did cocaine addicted individuals.
Multiple Sclerosis sufferers saw depression, fatigue and anxiety reduced, and the results were maintained at a 2-month follow-up.
Elderly patients found a significant improvement of their depression condition following neurofeedback treatment.
Surgery Residents with burnout and depression saw a return to a more efficient neural network following neurofeedback training.
Neurofeedback has been shown to improve sleep quality and sleep onset as early as 1982, with substantially more research interest confirming this in recent years, also in relation with pain and seizures.
Neurofeedback was shown to additionally benefit patients undergoing Cognitive Behavioural Therapy.
Motor Issues, Dyspraxia, Tics, Stutter, Tourette's
Our brain controls our movements. Functional connectivity dysregulation in autism can affect many of the brain areas involved in planning and executing motor actions. With neurofeedback, we can train these areas to improve symptoms in an evidence-based manner.
There are various cortical, and sub-cortical brain areas involved in motor coordination. With neurofeedback, we are training the cortex. Many cortical areas have deep connections to the basal ganglia and cerebellum, and it appears that we are training these deeper structures implicitly.
In our experience, the following issues can resolve with neurofeedback training:
– motor issues, such as dyspraxia and lack of coordination
– stutter and speech production
– facial tics
– uncontrolled, compulsive movements and actions.
Before and after brain maps corroborate these findings; research has so far focused on neuromarkers for these phenomena, and suggest neurotherapy as an adjunct to traditional therapies.
Tourette’s Syndrome can involve many of the above issues, as well as lack of executive control, again an aspect we have seen improve substantially with neurofeedback training.

Before and after brain maps corroborate these findings; research has so far focused on neuromarkers for these phenomena, and suggest neurotherapy as an adjunct to traditional therapies.
Tourette’s Syndrome can involve many of the above issues, as well as lack of executive control, again an aspect we have seen improve substantially with neurofeedback training.
Neurofeedback is an effective, evidence-based method to reduce migraines.
The source and phenomenon of migraines is elusive. Elements in the brainstem that form part of our reticular activating system are suspected to be generators. Neurofeedback training seeks to calm this.
Studies have found cortical differences in migraineurs, which gives us the opportunity to train relevant brain areas. Notably these comprise parts of the Default Mode Network, which we aim to strengthen with neurofeedback.
Personalised Brain Training takes a holistic approach and we look for comorbid symptoms such as PTSD, sleep issues, mood regulation, focus and attention, and anxiety to improve. Neurofeedback is an evidence-based approach to these challenges.
Migraines can respond quickly, though often the process can be extended; secondary symptoms such as sleep, mood regulation, focus and anxiety should respond meanwhile. This usually becomes clear within the first few sessions.
Obsessive - Compulsive Disorder
Obsessions and Compulsions are behaviour patterns we may observe, and which in themselves appear to be pathological or non-conventional. What underlies their motivation however can be far more sinister than what meets the eye. It is often a way for a person to manage or attempt to expunge an internal thought process, which they may or may not be conscious of. We look to break the cycle: Both the internal spiral and the physical manifestation (obsessive / compulsive behaviour patterns), which in themselves can precipitate further mental health issues and social problems.
There are different neural correlates for various OCD behaviours, confirming that this is not a unitary pathology. With a brain map, we can detect dysrhythmia, and train the relevant areas with neurofeedback.
Obsessive Compulsive Disorder is defined in the latest handbook of psychopathologies, the DSM-5, per below. For the purpose of seeking help and treatment with neurofeedback, a complementary therapy method, we are less interested in whether to fit someone in a basket – huge overlap may exist with other defined pathologies, which include depression, anxiety, body awareness issues, psychotic behaviour and the autism and schizophrenia spectrums.
Rather, we look for vulnerabilities as expressed in a Kaiser Neuromap and train these accordingly.
Comorbidities of OCD
OCD most commonly presents with a number of other mental health issues. With neurofeedback we can address most of these symptoms in an evidence-based, medication-free manner.
Around two-thirds of OCD sufferers also present with depression. One fifth have anxiety or panic disorder. Mood regulation, ADHD, trauma and substance abuse affects ten percent, as do body awareness disorders. Tics and autism can affect one in twenty.
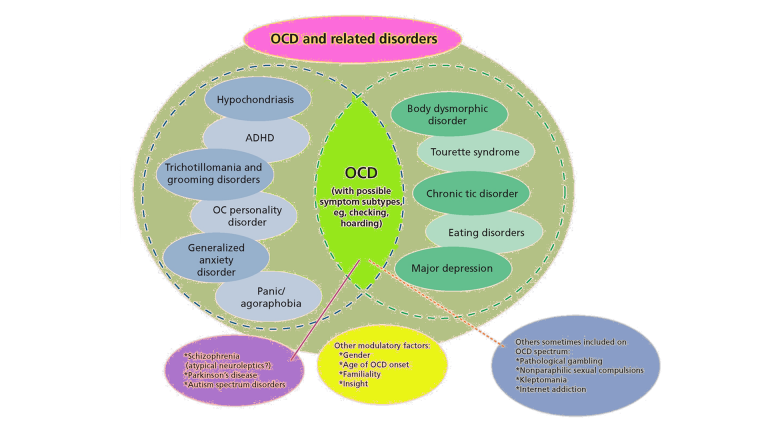
DSM-5 Definition of OCD
The presence of obsessions, compulsions, or both AND the obsessions or compulsions are time consuming (e.g., take more than one hour per day) or cause clinically significant distress or impairment in social, occupational, or other important areas of functioning AND the disturbance is not due to the direct physiological efects of a substance (e.g. drug of abuse, a medication) or a general medical condition AND the disturbance is not better explained by the symptoms of another mental disorder
(1) Recurrent and persistent thoughts, urges or images that are experienced, at some time during the disturbance, as intrusive, unwanted, and that in most individuals cause marked anxiety or distress; and (2) The individual attempts to ignore or suppress such thoughts, urges or images, or to neutralise them with some thought or action (i.e., by performing a compulsion).
(1) Repetitive behaviours (e.g. hand washing, ordering checking) or mental acts (e.g., praying, counting, repeating words silently) that the person feels driven to perform in response to an obsession, or according to the rules that must be applied rigidly; and (2) the behaviours or mental acts are aimed at preventing or reducing distress or preventing some dreaded event or situation; however these behaviours or mental acts either are not connected in a realistic way with what they are designed to neutralise or prevent or are clearly excessive.
Behaviour patterns we can seek to address with neurofeedback training include the following:
– excessive worries, intrusive thoughts and ruminations
– guilty ruminations and negative outlook
– preoccupation with self and appearance
– substance abuse issues
– inappropriate risk taking, impulse-control and lack of inhibition
– social awareness and invasive behaviour
– hallucinations, delusions and excessive internal dialogue
– repetitive restrictive behaviour
– letting go – emotional and physical hoarding.
Pain perception has neural correlates – there are brain areas that govern our attentiveness to the signs our bodies are giving us.
In the first instance, these signs are real messages that something is wrong and needs dealing with. Medical attention should provide solutions to this.
Sometimes, pain perception can become irrational in this context, and with neurofeedback training we can help the brain establish a more reasonable approach to interpreting such stimulus.
PoTS - Postural Tachycardia Syndrome
Postural Tachycardia Syndrome (PoTS) was first described in the 1940s, refined in 1993 and finally received a specific diagnostic code in October 2022. It is characterised by exercise intolerance and near syncope upon standing upright, elevated pulse (tachycardia) by 30-40bpm within 10 minutes of standing up, fatigue, anxiety and light-headedness. Often misdiagnosed as chronic anxiety or panic disorder, the group of symptoms comprised by PoTS has a biomarker and increasingly considered an autoimmune disorder, rather than only autonomic nervous system dysfunction. Specifically, increased levels of cytokines and chemokines characteristic of an innate immune condition were found, similar to autoimmune diseases like multiple sclerosis, psoriasis, type-1 diabetes, rheumatoid arthritis (RA) and systemic lupus erythematosus (SLE).
The condition affects females five times more frequently than males, mainly between 15-25 years of age, with over one million affected in the US alone. PoTS symptoms can persist for years, though half of patients find that orthostatic symptoms and functional impairment subside within five years, and of thost most within 1-2 years. It is estimated that 2-14% of Covid sufferers go on to develop PoTS, while 30% of long Covid patients, especially women, meet the diagnostic criteria.
A client presenting with PoTS like symptoms, recovered within three months of starting neurofeedback training, to the extent that the tachycardia was fully under control and anxieties had subsided substantially. Clinical studies will have to prove correlation. Notably, physical symptoms became manageable, from being previously incapacitating, in a relatively short period of time. This result is encouraging, especially with regard to the speed and extent of recovery, and neurofeedback has been shown to be effective for anxiety. Also, in this person, other neurological issues could be detected with qEEG.
Restless Leg Syndrome (RLS) affects about 5% of the population. It is a serious, chronic condition characterised by a painful urge to move the limbs. This is only relieved by walking, and can affect the ability to fall asleep, as much as concentration during seated tasks, like office work.
Treatment often involves medication that affects dopamine or norepinephrine levels. These are considered strong, regular and indeed permanent interventions by many.
Neurofeedback, in our experience, has woked in reducing and eliminating restless leg symptoms in many clients. In fact, while optimising training frequency during a neurofeedback session, the symptom has been observed to stop when this was found. A subsequent small deviation would restart the symptom, only to subside again upon return to the optimum training frequency. This suggests that restless leg syndrome is highly sensitive and susceptible to neurofeedback training.
To have a chance at permanency, it is recommended to do twenty sessions of neurofeedback. The cost of this compares very favourably to the irritation the untreated RLS causes. This includes lack of sleep, resulting irritability, loss of productivity, and the potential for side effects if a medication route is chosen.
Schizophrenia
Schizophrenia comprises a wide range of thought disorders, which ultimately affect an individual’s ability to share a reality with others. Causes can be trauma, emotional or physical; drug use; stress; genetics.
With neurofeedback training we aim to restore a healthy sense of self; flexibilise the social brain; and ameliorate comorbidities such as intrusive thoughts, mood disorders, focus and attention issues, paranoia and anxieties; and psychosis.
Neurofeedback training can improve functional connectivity and strengthen white matter tracts, both of which are impaired in Schizophrenia.
Each person is different: with a Kaiser Neuromap we assess individual vulnerabilities and train these with neurofeedback. Personalised Brain Training enables the person to unfold their genius in a socially reciprocal manner.
Neurofeedback is medication-free, non-invasive and evidence-based.
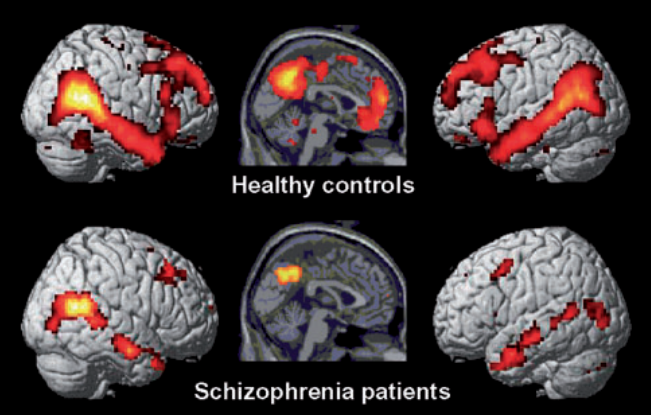
While there are certain commonalities between sufferers of schizophrenia, no two brains are the same. On the basis of a brain map we can identify particular vulnerabilities and work on these specifically.
Neurofeedback training can help restore the integrity of the Default Mode Network, the neural basis for ‘self’, as well as switching between self-referential states and active modes (the Central Executive and the Salience Networks).
Emotional self-regulation can be improved and anxiety, depression, sleep and focus issues alleviated.
Neurofeedback can calm the brain and help manage the ‘Voices’, as well as other regions prone to over-priming external agency. Significant reduction in Auditory Verbal Hallucinations (AVH) has been achieved with neurofeedback training.
Psychosis is a state that can occur, and recur, in persons diagnosed with Schizophrenia, Bipolar Disorder, Trauma and neurodegenerative conditions. Note however that it is not a necessary condition for any of these.
Daniel Webster of Neurofeedback London-Brighton has extensive experience working with Schizophrenia patients. Research and experience have shown effectiveness of neurofeedback training for Schizophrenia and its various comorbidities (see other tabs)
Psychosis
A feature of psychosis is a state of mind where all sensory stimulus is interpreted as being directed to oneself.
While it is natural for infants and children to interpret the world this way, we grow out of this mode between the ages of 3-5. We can assist this important maturation step with neurofeedback training.
As we mature, we start to learn that not everything that’s happening in the world is directed at ourselves.
Feeling as if everything is directed at us results in anxiety and / or deep depression, and clouds our interactions with others.
It also reduces our ability to take on other perspectives, consider different views and be accommodating of others’ stances. This reduces people’s self-awareness and thus insight into the need for change and improvement, providing another obstacle to betterment.
Shocks, such as trauma, drug use (in particular, cannabis and cocaine) and isolation (such as lockdowns) can cause us to revert into this child-like state, without us noticing.
Psychosis is a state that can occur, and recur, in persons diagnosed with Schizophrenia, Bipolar Disorder, Trauma and neurodegenerative conditions. Note however that it is not a necessary condition for any of these.
Schizophrenia comprises a wide range of thought disorders, which ultimately affect an individual’s ability to share a reality with others. Causes can be trauma, emotional or physical; drug use; stress; genetics.
With neurofeedback training we aim to restore a healthy sense of self; flexibilise the social brain; and ameliorate comorbidities such as intrusive thoughts, mood disorders, focus and attention issues, paranoia and anxieties; and psychosis.
Each person is different: with a Kaiser Neuromap we assess individual vulnerabilities and train these with neurofeedback. Personalised Brain Training enables the person to unfold their genius in a socially reciprocal manner.
Neurofeedback is medication-free, non-invasive and evidence-based.
Schizophrenia is an elusive term: its definition allows for wide subjective interpretation, and resembles almost an ‘other’ category for mental health disorders not elsewhere defined more strictly. Whether overlap and/or comorbidity, the following addresses the phenomenon resulting from dysrhythmia of key Default Mode Network nodes and thus a disintegration of the neurological definition of ‘self’. Labelling can have deleterious consequences for a person’s self-esteem, and it risks association with worse symptoms and manifestations than experienced.
In Schizophrenia, the formation of a neural basis for a ‘self’, the Default Mode Network, is impaired, as is its ability to anti-correlate with the Central Executive Network. Key nodes of these networks are often dysrhythmic, impacting the ability to self-sooth and self-nurture.
Thought disorders, delusions or hallucinations are signs of not engaging sufficiently with the outside world. These have neural correlates which we can detect with a Kaiser Neuromap and then train with neurofeedback.
Many other pathologies ensue, including trauma, mood dysregulation, sleep and focus issues, and other personality disorders are at risk of developing as the social brain breaks down.
With neurofeedback, we aim to restore social functionality, launching the person back into a virtuous cycle of affirmation and productivity with others.
Daniel Webster has done week-long intensives with clients, where substantial progress was made in reducing psychosis and trauma symptoms. This was ascertainable with before and after Kaiser Neuromaps, corroborating positive functional connectivity changes. These were confirmed cognitively by the clients and their families.
Neurofeedback is a form of complementary therapy and works alongside medication and psychotherapy, as well as calm-inducing approaches aimed at re-socialisation and maximising of interpersonal function.
Seizures and Epilepsy
One of the first discoveries made in the exploration of EEG, fifty years ago in 1972, was the ability to improve seizure resistance through neurofeedback.
An analysis of studies indicated that 82% of subjects demonstrated significant (more than 30%) seizure reduction, with an average value of 50%.
A 2009 review of studies established that EEG operant conditioning was found to produce a significant reduction on seizure frequency.
Barry Sterman was able to cure a 23-year old female epileptic from seizures using his SMR-biofeedback training over the course of two-and-a-half years.
Another pioneer of the field, Joel Lubar, reached similar results.
In our experience, neurofeedback has improved seizure resistant in many cases, and has always been beneficial in the treatment of secondary mental health effects. Medical attention should always be sought, and sources can be diverse and elusive.
Self-Harm
Impulsive aggression can become self-directed at times. This irrational urge is often triggered when an autistic child doesn’t get what they want, or feels misunderstood and frustrated. Self harm can also take the form of resignation, accepting less than one’s worth, and thus denying oneself recognition and opportunity.
Neurofeedback calms the mind and we can address brain areas contributing to self-harming ideation and intrusive thoughts.
We look to improve sense of self, reduce anxieties and strengthen inhibition levels while reducing self-directed impulsive aggression.
‘Self-harm’ can take many forms, and beyond physical manifestations (e.g. cutting, suicidal thought or even action) it can be more subtle:
– Accepting less than what we’re worth, overly and unnecessarily acquiescing to the perceived demands of others when not at all in our own self-interest, self-deprecation
– an inability to defend one’s own stance and needs are often overlooked and can be very harmful to a person’s development, especially when repeated and consolidated into a character trait.
With a Kaiser Neuromap we can detect vulnerability to such behaviour, including suicidal tendencies or ideation.
This is not diagnosis and it is non-specific in that dysrhythmia of the brain area(s) responsible for this is a necessary, but not sufficient condition. Nevertheless, it is a worthwhile finding that can help prevent worse outcomes by prompting awareness and intervention.
With neurofeedback training, we have helped self-harming adolescents transition from ‘cutting’ and dissociation to becoming engaged young individuals who are able to stand their ground, maturely deal with setbacks and embrace the sense of being part of a community.
Neurofeedback is a complementary therapy and medical attention should be sought in cases of self-harm.
Our brain interprets all sensory stimulus as directed to ourselves. We lose the ability to discern what is directed at us, and which matters or interactions are of no concern to us. This sets us up for panic attacks and ultimately psychosis. It also means we become singular in our perspective, unable to take on other points of view.
An extreme example is when we feel that too much is going on around us and we respond by having to turn the music down, explode at our environment or, potentially worse, retreating into tacit acceptance and self-deprecating thought. We can even feel that people are talking about us, and are convinced that we are the centre of every situation. This is highly stressful, resulting in anxiety and often deep depression. It can also lead to psychosis, for which this state of mind is a necessary, but not sufficient condition.
With neurofeedback, we can restore the brain’s ability to self-regulate efficiently.
Sleep
"I felt so calm last night! And slept like there were magnets between me and the bed. 10 hours straight."
"Slept like a log."
"Since I started neurofeedback training, my dreams have come back!"
Client testimony.
Sleep is where we recover – physically, mentally, emotionally.
It is a complex process whereby the brain enters different behaviour patterns in various stages. Slow wave sleep is where our body recovers; REM sleep is where we digest the day’s experiences, consolidate what we’ve learned and let our brain process memories and impressions.
Ideally, we would like to be able to switch off once comfortable, enter a deep sleep and wake up restored and energetic. If our sleep suffers, so do our concentration, productivity, physical abilities and emotional flexibility.
Neurofeedback has been shown to improve sleep quality and sleep onset as early as 1982, with substantially more research interest confirming this in recent years, also in relation with pain and seizures.
Brain areas and connections identified in research to be dysrhythmic in clients with insomnia respond well to neurofeedback training, in our experience, helping to restore REM sleep and depth of recovery.

Sleep is adversely affected by trauma and anxiety. First, the mind needs to ‘let go’ in order to enter deeper sleep cycles, which is a challenge for many. Excessive rumination and intrusive thoughts can hinder this, as does the loss of our ability to rationally calm ourselves down. The depth of our sleep is governed by our ability to self-nurture and create an emotional ‘safe space’. Homeostasis during various sleep stages is governed by other parts of our brain, some still involving the cortex. With a Kaiser Neuromap we can detect dysrhythmia in the relevant brain areas and train these accordingly with Default Network Training (together, Personalised Brain Training).
Focus and organisation suffers as a consequence of sleep issues. This time, different brain areas are affected, which we can also train. When we are unable to concentrate and produce our best output, we become demotivated and our mood and sense of self suffer. Again, there are brain areas responsible for these aspects of being, for which we can again detect dysrhythmia and provide neurofeedback training. The process is holistic – many components have to work together effectively for us to function optimally.
Neurofeedback has also been successful in treating other sleep disorders, such as somnambulism (sleepwalking), obstructive sleep apnea (to the extent the cause is not physical), confusional arousals, sleep terrors, nightmares, nocturnal enuresis (bed-wetting), delated sleep phase disorder, insomnia and restless leg syndrome. Evidence is provided at practitioners’ conferences and has yet to be manifested in published research. The above disorders have EEG correlates, which provides an intuitive basis for understanding that we have a chance at treatment with neurofeedback training.
Different neural hubs are responsible for sleep onset and depth of sleep. We can identify vulnerabilities with a brain map, and train these with neurofeedback to help restore healthy sleep hygiene.
Sleep is usually one of the first things to normalise during neurofeedback training.
We have also seen improvements in other sleep conditions, such as enuresis and sleep apnea.
Speech & Language
One in four persons with ASD are non-verbal, and 40% of all children referred to an autism clinic have significant speech delay, regardless of diagnosis.
Infants begin to understand and produce single words and gestures in the context of playful interaction from 12 months of age; between 18-24 months there is a rapid expansion in vocabulary and knowledge of rules regarding conversational exchange. Typically developing children will use language for social interaction; this contrasts with ASD children who are more likely to use words to regulate their environment (demands, protest), rather than with communicative intent. Despite the range of language abilities, articulation skills are generally spared. There is a strong link between language and social skills in autism.
Speech development has numerous components, all of which have neural correlates, meaning there are brain areas contributing towards language comprehension and generation, which have to mature and work together efficiently. This means we have a chance to improve speech generation by training the brain, and both research and experience confirm this. The research below illustrates how we can assist with improving necessary building blocks that contribute to a person’s development of speech and language capabilities.
Speech and language development are also a function of social reciprocity, both with regard to initiation and reception. It should therefore not be seen in isolation, and rather as an accompanying component of improving effective synchrony with the social environment.
Personalised Brain Training takes a holistic approach to improving social integration by way of training various features of cognition and consciousness, including sense of self, joint attention, Theory of Mind, focus, mood regulation, behavioural challenges and communication, both verbal and non-verbal.
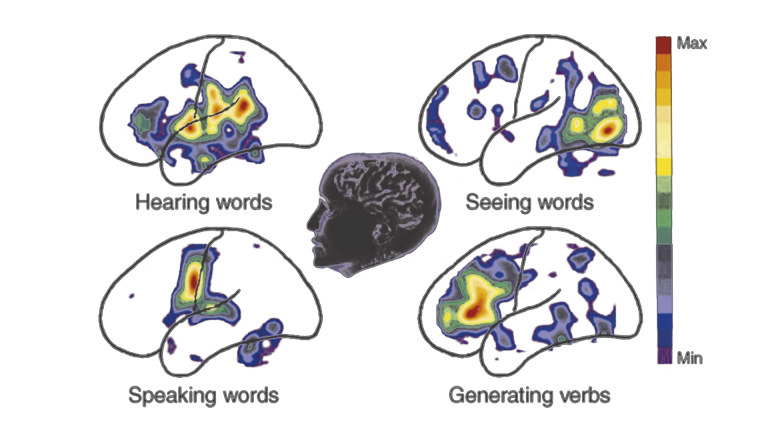
Research on Neurofeedback and Speech
Neurofeedback training was shown to improve speech-in-noise perception and auditory discrimination that was applicable post training and long-lasting. This shows that we can positively affect neural encoding of acoustic inputs in the auditory cortex, a frequent issue with autistic individuals.
In ADHD children, neurofeedback training improved visual memory, enhanced auditory short-term memory and auditory working memory.
Biofeedback produced better and more lasting effects than traditional therapy in behavioural dysphonia.
Neurofeedback was shown to improve the ability to identify emotional prosodic intonations.
Phonetic recognition and reading skills have been shown to improve with neurofeedback training, another important component of speech and language acquisition (see “Dyslexia”).
Personalised Brain Training is a holistic approach; we also train brain areas relating to focus, motivation and sense of self, as well as sequencing and motor skills, all of which contribute to the development of speech.
Training and Intensive Courses in the UK and Internationally
Daniel Webster offers the most advanced neurofeedback methods as home visits and intensive courses, in the UK and internationally.
Most clients find 10-20 weekly sessions produce transformative results. Sleep improvement, and a feeling of emotional groundedness tend to emerge within the first few sessions. The training effect quickly builds up as we address brain areas responsible for regulating mood, motivation, attention and focus, and our ability to regulate physiological arousal. Anxieties subside and social interaction takes on new dimensions. We feel valued, able to express our unique skills and strengths, and performance improves, paying dividends on the investment in Personalised Brain Training.
Intensive courses involve two sessions per day over the course of a week or longer. Transformative results can be achieved in a short time period, where we accomodate 10-20 sessions in the UK or internationally. Children enjoy the exceptional screen-time during their school holidays, balanced with activities in and around London. Adults find this a similarly efficient use of time off work, combined with a trip to a new location, and gain additional confidence from negotiating novelty and finding acceptance in a welcoming environment, providing a more effective re-set.

Hybrid courses involving intensives and weekly training are a convenient way of achieving faster results, utilising term breaks and vacations, or long weekends.
There are distinct brain areas that interpret the respective sensory input, and through various convergent processing stages – multi-modal association areas – the brain constructs a scene, and understands where we are with respect to our environment. When any of these brain areas becomes dysrhythmic, our interpretation becomes distorted, for example, we can become hyper- or hyposensitive, as is seen in various symptoms of autism spectrum disorder (ASD). This is an extreme, and we all operate on a spectrum with regards to cortical functionality.
With neurofeedback, we can train the brain areas relevant for efficient sensory processing and integration. Personalised Brain Training uses the most advanced qEEG brain map interpretation method to form an individualised training plan. Our neurofeedback method applies the most effective training protocols with an enjoyable feedback process, watching movies of choice.

Sensory processing is a well-researched process that involves many dedicated brain areas, and their interaction to produce an impression of our environment, and how it relates to us. Higher integration of ensuing awareness leads us into the realm of “what is consciousness”:
Science shows that our brain is engaged in a constant process of modelling, or predicting, our environment, both with regard to space and time. It does so on the basis of previous sensory information, as well as recent and consolidated memory. Predictions are then matched with reality, and the process begins again. This is an important distinction from the idea that we are merely reacting to our sensory input. It introduces the theory that we essentially anticipate the next moment, and then update our model of our environment, continually.
The neural correlates of this is our Default Mode Network, a system of brain areas that work together to provide a neural representation of self – a state we enter upon self-reflective thought or imagination. This set of nodes activates counter-cyclically to our Task Positive Network, key association areas that interpret our sensory input and plan and execute actions. When this clear, cyclical separation is inhibited, our predictive capacities become impaired and we lose synchronicity with our environment. With neurofeedback, we can train this non-sensory specific brain functioning as well.
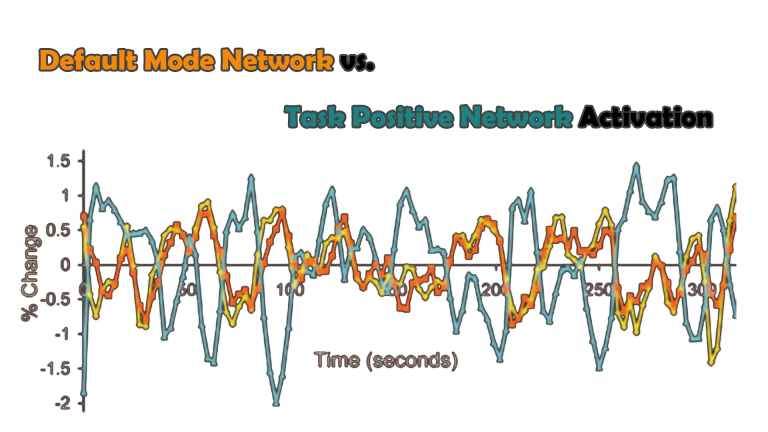
Case Studies
Deirdre’s daughter Monica, 10, suffered from severe intractable epilepsy, with up to twenty awakenings due to heavy seizures in a night. While working with Monica, we also did neurofeedback training with Deirdre. Effectively in a state of constant alert and hypervigilance, Deirdre had a strong grounded personality, which showed in her brain map. Nevertheless, the physical and emotional strain was taking its toll, in particular on her sleep, and consequently her ability to focus on her writing project, while managing an impending divorce and relocation. Within the first sessions, her sleep improved substantially and she felt more productive.
"I felt so calm last night! And slept like there were magnets between me and the bed. 10 hours straight."
"Slept like a log."
"Since I started neurofeedback training, my dreams have come back!"
Client testimony.
Lorna had enjoyed what from the outside appeared to have been a privileged life, having enjoyed private education, a lucrative and indeed fulfilling role in the family business, and accumulated some reserves. She had been medicated for bipolar disorder and ADHD from the age of eight, in what she felt was a suppression of her bubbly personality that didn’t conform to parental expectations of ‘order’ or ‘normal’ behaviour. She had always been social and outgoing, enjoyed boarding school, yet she now felt things had come to a head and that she was not living to be the person she could be. Instead, she believed she had conformed to the wishes of her family and ignored her own needs, emotionally, socially, and fundamentally with regard to her identity. Mood swings, disturbed sleep, lack of focus and self-critical thoughts deprived her of joy in her life. As opposed to deprivation of nurture, Lorna had been domineered by her parents, and not been able to develop her own sense of self-nurture. Her identity and sense of self worth were shattered.
Within five sessions, Lorna’s sleep improved noticeably, as did her energy and motivation. She enjoyed doing long sessions, in particular the film “Now, Voyager” with Bette Davis reminded her of her upbringing and situation. After ten sessions, Lorna began working with a talk therapist to reorganise her life and ambitions – teaching in India was a dream she thought could be realised. Her sense of despair had disappeared, and yielded to a slightly overly self-conscious anxiety, which was the first step past numbness. Lorna’s productivity improved and she began to set herself higher goals, leading to some frustration, yet this substantially contrasted with her previous despondency. A further few sessions helped with the self-blame and internal chatter, and Lorna is on a good trajectory.
Maria, 77, an avid reader, discovered in her 60s that she had an irreversible eye condition, a glaucoma, that was causing her tunnel vision. She was able to stabilise the development with medication, yet it led to a few nasty falls, one of which left her concussed. A Kaiser Neuromap showed the expected areas of brain hypometabolism, and we trained her accordingly. Ten sessions later, her sleep was restored, as was her perceived memory, and a remap showed that the brain areas had responded. She felt more productive and grounded and enjoyed the experience of watching multiple movies, her favourite being with Audrey Hepburn.
Marcus’s wife had suspected that certain of his mannerisms had changed, he had become more impulsively aggressive at minor things that changed his routine, and she believed his gait had changed, beyond the mere effects of working from home for the last, stressful, two years. Socially withdrawn, Marcus was focused on his consulting work which had started to pick up again. The joy in his life was lacking, despite having a supportive family.
A brain map revealed some unusual areas of hypometabolism, that would warrant further investigation into whether they are early signs of neurodegeneration, possibly Alzheimer’s Disease. There are certain non-specific neuromarkers, as well as expected reduction in functional connectivity of the corpus callosum that joins the two brain hemispheres. We also found signs of emotional stress and a tendency to internalise, and excessively blame oneself. Two neurofeedback sessions based on these findings returned Marcus’s sleep to a level he had forgotten existed. He became more focused on his work and related social interactions, and had the best financial year of his career.

Linda had been betrayed by her husband. The realisation set in just before her fiftieth birthday. In her second marriage, living in her dream house with an eleven year-old daughter, she felt vulnerable and despaired. They had gotten through the lockdowns as a family, while her social life suffered, and she no longer felt her bubbly self. On top of this she was going through menopause, a disorienting experience, and her daughter was striving for teenage independence in a most hurtful way. Linda had experienced depression before, tried every medical and alternative healing path, and even been to rehabilitation as a way of setting a line to her partying lifestyle in her twenties (“rehab doesn’t work. I’ve made great friends there though!”). She knew there was a resilience in her, which after all had enabled her to transition from being a single mother with an insecure singing career to affording her current lifestyle and the stability it represented. This was now shaken.
Self-doubt and introversion were not her natural habitat, yet she felt isolated, and even began to think she had incurred brain damage as a result of her youthful excesses. Linda was taking anti-depressants and immersed herself in a temporary sales role, which had just come to an end. With time on her hands, she decided to try neurofeedback training.
Visibly nervous excitement before the first session quickly subsided. We started with a brain map, and just wearing the shower cap-like recording device made her feel calm and sleepy. This takes about half an hour, and we quickly proceeded to do a first training session. The cap is replaced with three sensors gently fitted to her head at the areas we look to train. Settling for a Robert de Niro film, Linda was quickly immersed, relaxed and amused. The morning passed swiftly and she was on her feet ready to pick her daughter up for school after the session ended. She noted that her sleep was particularly deep that night.
Linda’s brain map showed substantial deactivation of her prefrontal cortex, something she worried was a result of historic substance abuse. A remap after ten sessions showed visible improvements on this metric, as encouraging as her other improvements in mood, focus and self-confidence.
Intrusive, self-critical thoughts subsided and her motivation returned along with focus and deliberation. She felt particularly productive after each session, and this gave her great confidence. Changes were apparent in every way. Even her husband was amazed – “you’re back to your bubbly self!” Linda began feeling a healthy sense of detachment, and was no longer lifting the weight of the world by herself. She had gone from being reactive and despondent to taking control and setting the rules, which her husband obligingly acquiesced to.
A former singer in a band, she started humming tunes to herself again, and there was music playing in the house, replacing the solemn silence that was deafening upon our first meeting. Soon, projects began, she replaced artwork in the living room and began some redecorations.
Being on her own was no longer her refuge of choice; instead she rekindled productive relationships, and set aside people and places that were soaking up her energy. Her schedule filled, as she accomplished her spinning workouts before our sessions, and project partners were waiting outside as we finished.
Linda started to accept her marital situation, redeemed her sense of self-worth, and found a way to make partnership and parenthood work beyond traditional confines.
Her brain map corroborates the transition: previously absent alpha peaks emerged visibly, mirroring the cognitive resuscitation she was experiencing. Other vulnerabilities in her initial brain map included:
- mood control;
- lack of emotional safety, or feeling ‘underloved’, both by family and the world at large;
- heightened auditory sensitivity and a tendency to over-attribute emotional content into how things are said;
- focus and planning issues;
- various anxieties – “what’s next”, social anxiety, a sense of everything being directed at her, hypervigilance, and emotional betrayal
- disengagement from her surroundings.
Linda did twenty neurofeedback sessions, over the course of seven weeks, usually three per week. During this time, she had dropped the use of anti-depressant medication (in consultation with her prescribing GP / medical doctor). We did a remap after ten sessions, which showed substantial changes in her overall brain activation and guided the next ten sessions. (She had already commented, “It’s worth it!” after session five). After twenty sessions, Linda’s perceived transformation was corroborated by her final brain map. Of particular note is the way her immediate family embraced the changes, as her daughter began confiding in her.
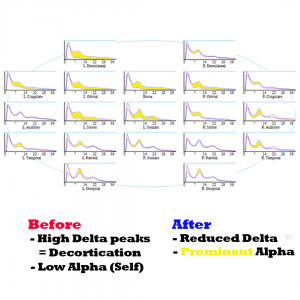
Anna was prone to strong intra-day mood swings as well as having endured a manic episode, during which she became the subject of financial and emotional exploitation. Importantly, Anna was not psychotic; however she suffered from strong attachment disorder, fear of abandonment, some social awkwardness as a result of an impaired sense of self, and lack of ability to rationalise emotions, despite her warm demeanour.
Following a particular slump triggered by betrayal, and being subject to physical violence, she began neurofeedback sessions. Her sleep improved immediately, as did her outlook. Within five sessions, she had become her usual optimistic self again, and began looking for a new vocation. Within weeks, she had a new job that combined two of her passions and talents, and on a solid path to recovery and forgiveness.
Anna’s mood regulation has substantially improved during her ten overall sessions; she feels more grounded and motivated, while enjoying the cause of her work and the new people she is meeting.
Stephanie, 40, had recently suffered numerous destabilising incidents and conditions that deprived her of her joy of life and made everything seem extremely stressful. One night while preparing dinner, a confluence of her husband’s criticism, her kids screaming and the music on the radio overloaded her senses and she smashed a plate in desparate frustration. It was as if everything was directed at her, and her mood swings and lack of emotional support exacerbated the erosion of purpose she had come to feel. The previous years had deprived her of both parents, and she had ceded freelance work to raising her small children and looking after her ailing mother. Next-door building work continued throughout lockdown, and the family was on the constant verge of deciding to move. Furniture and clothes were packed, and the idea of nesting could not seem more remote. Stephanie felt under constant assault while not progressing personally or professionally. This strain entered her previously strong relationship with her husband, himself under substantial work pressure. Having self-diagnosed as PTSD, both decided to do twenty neurofeedback sessions.
Within a few sessions, Stephanie’s sleep was restored, and she became more motivated and relaxed. It no longer felt as though everything was directed at her, and she was able to respond to unexpected outcomes flexibly and with humour. This did wonders for her relationship, and she felt her children sensed this too. A brain map confirmed this progress.
Mary, 35, had contracted Covid in January and had almost been hospitalised. Six months later, she was still working part-time from home and felt like a shadow of her former self.
She was suffering from fatigue, anxiety and depression, and her sense of smell had not recovered. Brain fog, which could also be attributable to her perimenopausal stage, significantly reduced her productivity and confidence.
Mary’s sleep improved from the first neurofeedback session, as did her physical stamina.
Within three weeks, or five sessions, she noticed her sense of smell had begun to return.
Motivation and focus improved substantially through session ten. Mary felt reinvigorated and her self-critical thoughts subsided. “I’m there for my family again!” she commented.
We did another seven sessions, now spaced weekly, during which Mary remarked that she had never felt a clearer mind before.
It is not suggested that neurofeedback is a “cure” for issues arising from a Covid infection, and we will never know what caused her sense of smell to return. However it was reassuring to see how Mary’s general sense of self and well-being had improved during the time we were training.
Camilla had been diagnosed with anxiety, panic attacks, associated insomnia and mild depression. She was prescribed two anti-depressants – Mirtazapine and and SSRI – which she was able to reduce to a minimum dose over time. During the last three years however, she had six relapses, each following a similar pattern: Stress (emotional and work-related) and fatigue precipitated intrusive thoughts and worries, setting off a familiar path of insomnia; consequently higher anxiety, increased stress levels leading to panic attacks and depressive symptoms. The first few episodes were stabilised by resuming Mirtazapine, which helped restore sleep. The subsequent ones however failed to respond, taking months to stabilise sleep and reduce anxiety, which involved having to take time off work. In addition, she began to have somatisations, beginning in the spine and ultimately reaching her face. Migraines began to reappear when she became excessively tired.
Guided by a brain map, we began doing neurofeedback training twice a week. Camilla’s sleep became sound after the second session – “I feel pleasantly knocked out” – and she decided to reduce her Mirtazapine dose gradually in accordance with her prescribing GP. After eight sessions (four weeks) she was on the lowest dose, and even this left her feeling very groggy in the morning. Camilla had regained confidence in her ability to fall asleep, and stopped using Mirtazapine completely. Her anxiety levels were at their lowest, and she had began to work again, leaving a corporate environment to work with children in a mental health setting – a stressful yet engaging and meaningful activity. Her motivation had reached new levels, and she felt stable and confident, which showed in her stance and demeanour.
Ten sessions of neurofeedback training (each two hours) were sufficient to stabilise Camilla, restore her ability to sleep, and the confidence therein, as well as improving sense of self-worth, focus and motivation. She has not felt the need to use Mirtazapine again since.
Three months later, Camilla reports a major improvement in how she is able to set boundaries, both at work and in her personal life, and not neglecting her own well-being.
Janet, 56, was bursting in her every capacity – as mother of two teenage daughters, wife of a Long Covid-suffering income producer, daughter of an ailing mother with dementia, sister of a libertarian, care-free brother whose involvement with his kids contrasted starkly with her own, friend of contacts she had not had for three years since lockdowns, and undergoing her own menopausal transition.
She had spent the first term of the school year under severe stress, committing herself fully to support her two adolescent daughters, and inserting herself further into every fibre of their lives. She acknowledged that this was the reverse of how her brother was managing his children’s transition into early adulthood. Her own sleep had not been great to start the term with, and the built up worry, anxieties, and pre-existing mood control issues were exacerbated by the stress. Afraid of losing control, and the pending next stage of her own life once her children were going to go to university and leave the house, she compensated with surrendering any own motivations to perceived helpfulness and dedication.
Janet’s career as a casting director had been put on hold when she met her older husband John, whose banking career enabled them an adoption of two infant girls as she was infertile due to an autoimmune condition. In perceived competition with John’s two adult boys from a previous marriage, the girls were enlisted in the same schools. Insecurity and racism plagued their early upbringing, and they were now completing their Six Form (11-12th grade) in an acceptable private school. So big had the strain been on them, along with individual trauma, that both had mental health issues we resolved with neurofeedback training before and during term.
Janet had developed a paranoid cynicism that preceded all social interactions, as if to purposefully conjure up antagonistic reactions in an attempt to prove the worst and thereby achieve some sense of control and certainty. She was ever more convinced of intrinsic racism and antagonism towards any of her causes, and complained about the abolition of social distancing and other Covid measures that had happened over a year ago by now. Her overbearing intensity was difficult to dispute, and it appeared that her children, and husband, were suffering from her lack of self-insight. She would frequently break down when out of sight of her children, upset when her husband, himself suffering from Long Covid symptoms, found the occasional energy to call her ‘neurotic’. It would take a year after her daughters for her to commence neurofeedback training for herself.
Unlike her daughters, and her husband, Janet found it difficult to even tolerate opinions and views other than her own. Any perceived opposition, no matter how well-meant, would trigger her, and she had a tendency to infer the worst. Physiologically aroused, she would immediately turn combative and seek to quell any source of dissent or alternative point of view. This inflexibility applied to the most mundane of issues, such as changes in recreational plans for the day, to political views and current affairs, as well as deep-rooted convictions regarding the Covid pandemic and its resolution, which was being handled completely unsatisfactorily three years after the first lockdown. Janet’s autoimmune condition made her feel particularly vulnerable, and to her, masking and social distancing provided the minimum necessity in public interactions. She saw herself as the only agent of sense and pragmatism in her household, and therefore set the rules. The family was confined to isolation from the first lockdown. Physically, they were staying at home and not going to restaurants theatre shows as in the past. Socially, movements and interactions were severely constrained and limited to family outings. Meetings with friend were rare and heavily vetted, in particular with respect to Covid protocol observation but also perceived sense of responsibility. Volunteering projects, birthday parties and even cinema outings were off-limit. Living between two homes, both far from school and other classmates, furthered this separation. Her daughters were meanwhile the only ones in their class to wear N95 facemasks at all times – a condition that eventually got relaxed regarding outdoor breaks. Janet was driven by her perceived need to be involved and in control.
As a result, Janet was finding it difficult to feel part of something bigger – the outside world had firmly conspired against her, and from a neural perspective, this caused great instability. Her moods were also subject to violent, and fast, swings. Smiles and motivation could cede to despondence and crying in despair within a few hours. It was as if her fighting spirit was the only thing that could fire up her will power, at great emotional and energetic expense. Combat was her main driver, and she would find antagonism in anything and everyone, any fault triggering a polarised perception. School provided an outlet, as she got involved in every any aspect of her children’s education, trying to impose mask mandates there and actively communicating with teachers about coursework and teaching methods. Only parents with common grievances were part of her circle, and still this fluctuated by topic.
Unable to fall asleep easily, she would research the internet late into the night, and she was woken up easily at any time. Janet’s mind was racing at all times, and she felt like she was having to defeat internal voices of dissent when left to her own devices. She had long felt a dissociation from her body, and couldn’t remember the last time she had been given a hug. Her daughters’ growing desire for independence, and the prospect of complete solitude once they would graduate in a year’s time, frightened her. She was distrustful of medical doctors, especially as most had ceased to wear face masks, and had only one (paid) confidant in form of a psychotherapist who was willing to agree with her on everything.
Janet’s obsession with “wanting to be there completely” for her daughters’ final two years of school was placing a burden on her environment. She was at war with the headmaster, in particular regarding the laxer Covid protocols; teachers, concerning their methods and interactions; society at large for the cessation of vigilant pandemic measures she considered premature; her husband, whose despondence she could not attribute to her domination on all issues; and even her daughters’ search for privacy and independence, which she took personally in a highly emotional manner. Seemingly well-intentioned, her actions were socially disruptive. On a long-awaited family summer vacation, she prevented her daughters from mixing with peers out of fear that they would be drawn into illegal activities that the law would interpret differently with respect to them due to their ethnicity. Dinners were cut short when she felt others’ views were out of order, a frequent occurrence. Her daughters were showing signs of strain throughout the summer, one threatening self-harm and the other suffering from panic attacks. Both overcame their challenges with neurofeedback training.
Janet’s body began to give. A year after her daughters’ neurofeedback training, driven by the same ideals and obsessions, Janet began to experience cardiovascular issues. Heart dysrhythmia was diagnosed and treated with medication. She found it difficult to accept the advice of rest and detachment. Thoughts became intrusive, and even her therapist found the courage to voice their concerns about her trajectory to her. It was just before Christmas that she decided to reach out for neurofeedback training, whose success she’d witnessed in both her daughters.
We began with a brain map, which confirmed her relational thinking, mood and sleep disorders, various trauma markers, and sources of anxiety. Knowing, and fearing, that “this could change me”, we talked through the findings, which have an objective nature due to being based on physiology, or observed functional connectivity between brain areas, rather than being a subjective award of pathologies by an authority, for most of whom she harboured deep contempt. The fear, “could this change me”, had already been objectively overcome with her commitment to an initial brain map and session; subjectively, the prospect of achieving better sleep and reduced internal chatter had become sufficiently appealing.
As a former casting director, Janet retained her interest in art and theatre, and chose her favourite films to watch in session. Quickly engaged with the content, sessions felt non-invasive enough for her to tolerate. Neurofeedback sessions obviated the need for overt introflection, by contrast to talk therapy, and avoided triggering her with the result of reanimating her combative style. Her views were not questioned, and her brain trained to achieve a healthy sense of detachment in the first instance. This took a few sessions, during the course of which she noticed her sleep improving drastically. Being able to let go of her thoughts at night and settle into a deep state of relaxation was previously a feared scenario, yet this began to feel more natural and energising with every session. After five sessions, she noticed how her behaviour and reactions had began to change. No longer anticipating the worst in every situation, she felt a calm optimism and motivation that she could not recall having experienced for a long time. Relations with her supportive husband improved to everyone’s relief, and her daughters’ were positively surprised by her evolving lack of invasiveness. For the first time, it appeared that Janet was able to recall her own frustrations in her childhood at being micromanaged by her parents, and share this admission with her family. To everyone, it felt as if a weight was being lifted.
Encouraged by the positive feedback from her immediate environment, Janet continued with weekly neurofeedback sessions. At one point, she felt particularly emotional after a session, and found herself confiding in her brother on a long phone conversation that night. She felt lighter as a result, but was plagued with some remorse and guilt about how she had been acting. A supportive environment helped her achieve self-forgiveness and a more positive outlook. Reminded of her progress, she drew strength from the shape of her changed trajectory. It was as if people started to come closer to her, piercing an invisible wall she had built up around herself. Janet began to feel part of a social fabric that had an enabling quality and created a source of stability. Her moods and motivations became more stable, and she resumed interests in art that she had parked long ago. Within two months, Janet was talking to people from previous work-related circles who encouraged her to resume projects she had previously excelled in. Meetings followed, and melded into a social life. Physically, Janet felt better rested and ensconced in her body; hugs mattered, and her sensitivity was reciprocated. Embedded in a supportive environment, Janet began to flourish. Intrusive thoughts became ideas, and fears turned into surmountable challenges. She wished that she had begun training earlier, in parallel with her daughters, and was now living in the moment.
Neurofeedback is a form of complementary therapy and should not be seen as a replacement for conventional medicine. qEEG brain map-based neurofeedback training takes a more holistic approach to brain functioning, rather than just focusing on medical symptoms. It is not intended as a form of diagnosis nor medical intervention nor medical advice per the disclaimer.
Brain Maps and Personalised Brain Training Explained
Personalised Brain Training with Neurofeedback
Neurofeedback lets us train dysrythmic brain areas. With sensors comfortably fitted to the brain areas we want to train, we detect brainwave patterns real-time while watching a movie. When these patterns are inefficient, the volume drops momentarily. This is the feedback we are giving our brain, short and instantaneously.
The brain area we are training recognises this – while our conscious mind is focussed on the movie – and adjusts its behaviour to restore the normal volume. With repetition, throughout a session, learning occurs.
Meanwhile our conscious mind is solely focussed on the movie; the training process is passive in this sense.
The drop in volume is subtle, so we continue to understand the flow of the movie. No current or electrical stimulation is fed to the brain; sensors simply read brainwaves and the feedback is purely audio-visual.

Neurofeedback trains our Pre-Conscious Mind
Rather than engaging the conscious mind, which slows us down, we are training preconscious processes.
This equips us with the ability to live in the moment and attain our potential (if we have to resort to conscious control, we are not living in the moment).
We take a holistic approach to healthy brain self-regulation, rather than categorisation or diagnosis.
Personalised Brain Training is an advanced qEEG brain map-based approach to neurofeedback training developed by the founders of the field. Taking Othmer Method / ILF training methods further, it employs Default Network Training protocols as developed by David Kaiser.

Neurofeedback is Evidence-based
Neurofeedback training is an evidence-based complementary therapy. Its efficacy was first demonstrated some 50 years ago, and with advances in technology, training protocols have become more efficient and the feedback method – watching movies – thoroughly enjoyable.
Neurofeedback is evidence-based. It’s first application was discovered in 1971 when it was used to resolve intractable epilepsy.
There are over 2,000 peer-reviewed research reports on PubMed demonstrating efficacy across a number of pathologies.
In the US, it is an accepted complementary treatment for many challenges.





